John was sitting in his deer stand in Mississippi when he first noticed a small lump beneath his jawline.
At 69 years old and a practicing pharmacist with more than four decades of experience, he assumed it was nothing serious, likely just a lymph node still reacting to a recent respiratory virus.
“I had just kind of gotten over a sore throat a few days before,” he says. “I figured it was probably a lymph gland inflamed from the sore throat.”
But a few weeks went by, and it didn’t go away. So, he walked next door to see his friend, an ENT physician, who took a closer look with an endoscope.
“He said, ‘Man, your tonsils on that side are three times the size of your other side,’” John recalls. “He couldn’t really tell what was causing it, so he told me to take antibiotics for 10 days and come back if it didn’t get better.”
It didn’t. A scan followed. The results were concerning: probable metastatic lymphadenopathy. Likely cancer.
At that point, his ENT friend recommended seeing a specialist, and one who uses advanced robotic techniques. A few days later, John had an appointment with Sagar Kansara, MD, otolaryngologist at Our Lady of the Lake in Baton Rouge.
A New Kind of Surgery, A Better Option
Dr. Kansara confirmed the diagnosis: HPV-positive tonsil cancer. HPV-related throat cancers are increasingly common, especially in men over 50, and are typically more treatable than other types.
John was presented with two treatment options: radiation therapy or surgery. More than anything, John wanted the cancer gone, and he chose surgery.
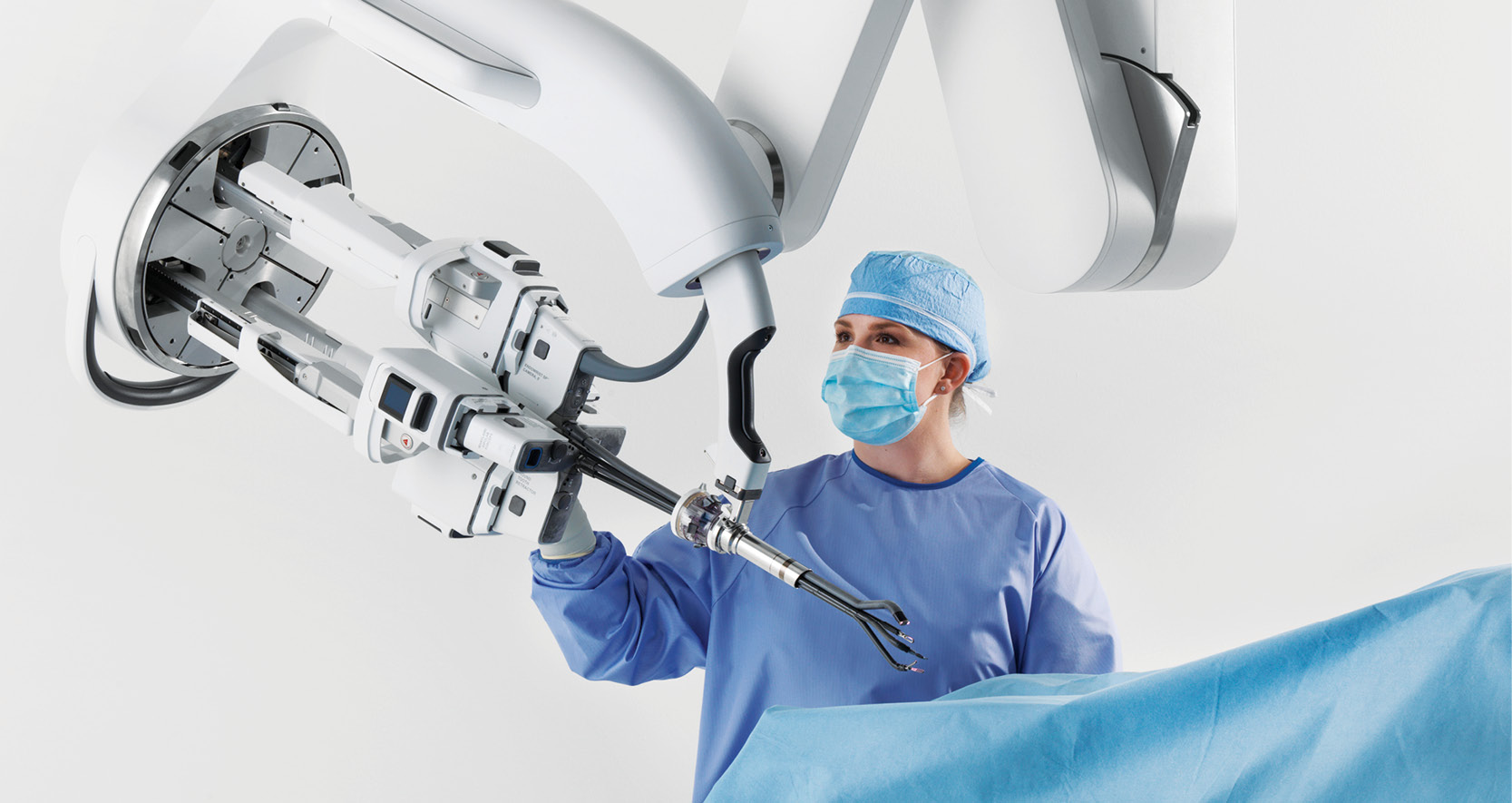
Dr. Kansara used a minimally invasive technique called Transoral Robotic Surgery, or TORS. This method uses robotic tools inserted through the mouth to remove tumors in hard-to-reach areas like the tonsils and back of the tongue. The approach avoids external incisions, reduces trauma to surrounding tissues and helps patients heal faster.
“He removed my tonsils and then also checked all four different levels of lymph glands, a total of 23 or 24, maybe more,” John says. “The only one that had any involvement was the one directly associated with that tonsil. All the rest came back clear.”
Clean margins. No signs of spread. And a pathology report confirming that he was likely cancer-free.
“We even did a tumor marker blood test a few weeks later to confirm what we thought, and it came back negative, too.”
Faster Recovery, Fewer Side Effects
For many patients, TORS means a much smoother recovery. John says he was back to his normal routine in just a few weeks, something that surprised even his friends.
“After I had the surgery, I found two or three people within a couple of weeks who had [similar diagnoses]. Their experiences were not nearly as good as mine,” he says.
Some of those patients, he says, lost 30 to 40 pounds and had recovery times of six months or longer. “I think I lost 10 to 15 pounds over about three weeks. But it’s gotten better, significantly better.”
He stayed in the hospital two nights, took no prescription pain medicine after discharge and was eating soft foods like scrambled eggs and grits within five days.
“After a couple of weeks, I was kind of good to go,” he says. “And now I’m sitting here talking, and from a feeling perspective, I wouldn’t even know I had the surgery.”
A Care Team That Stands Out
From start to finish, John says the care he received at Our Lady of the Lake exceeded every expectation.
“Dr. Kansara is just wonderful. And the reason he’s so successful is because this is what he does all day, every day. That’s why it’s critical to go to somebody like him, or him specifically.”
He also gave high praise to Dr. Kansara’s staff for their compassion and patience throughout the journey. The personal touch, John says, made a hard situation feel a little easier.
“From the actual surgery to the surgical team to the hospital, I can’t say enough good things about the whole experience,” he says.
Looking Ahead: ‘I wouldn’t change a thing’
Now cancer-free and back to daily life, John said he’s grateful for both the outcome and the way everything was handled along the way. Though John works just 75 yards from one of the largest medical centers on the Mississippi Gulf Coast, he didn’t hesitate to drive to Baton Rouge for his care. And, he says, he’d do it again in a heartbeat.
“It was really a best-case scenario from a disease perspective and from a surgical perspective,” he says. “I’m pretty much, you know, back to normal — swallowing, talking, eating, that sort of thing. It’s really been a best-case scenario.”
He credits the robotic approach and Dr. Kansara’s experience for how well it all went.
“The trauma is significantly less from robotics,” he says. “The old school way was much more invasive. And so yeah, I certainly contribute my speedy recovery to the robotic procedure and to the skill of Dr. Kansara.
“This was the right decision. And I wouldn’t change a thing.”